Management of Tinea Corporis
Definition of Tinea Corporis
The term tinea corporis refers to dermatophyte infections of the trunk, legs and arms, excluding the groin, hands and feet.
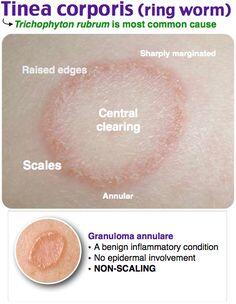
Clinically, tinea corporis often presents as one or more annular ("ring-shaped") lesions with a raised, scaly border and central clearing. Mild itch or discomfort is common, and lesions may slowly expand if untreated.
Geographic Distribution of Tinea Corporis
The condition occurs worldwide, but it is most prevalent in tropical and subtropical regions.
Warm, humid environments, crowding, and close contact with infected people or animals can facilitate spread. However, cases are also frequently seen in temperate climates, particularly in settings such as schools, day-care centres, and households with pets.
Causal Organisms
Tinea corporis is caused by E. floccosum and many species of Trichophyton and Microsporum. Infection with anthropophilic species, such as E. floccosum or T. rubrum, often follows autoinoculation from another infected body site, such as the feet. Tinea corporis caused by T. tonsurans is sometimes seen in children with tinea capitis and in their close contacts.
Tinea corporis commonly occurs following contact with infected household pets or farm animals, but occasional cases result from contact with wild mammals or contaminated soil. M. canis is a frequent cause of human infection, and T. verrucosum infection is common in rural areas. Tinea corporis is more common among individuals who have regular contact with animals or soil. Human-to-human spread of infection with geophilic or zoophilic species is unusual.
Determining whether infection is due to an anthropophilic, zoophilic, or geophilic species can help identify likely sources of exposure and guide preventive advice for the patient and close contacts.
| Organism type | Examples mentioned | Typical exposure pattern |
|---|---|---|
| Anthropophilic dermatophytes | E. floccosum, T. rubrum, T. tonsurans | Autoinoculation from tinea pedis or other body sites; close contact within households or among children with tinea capitis |
| Zoophilic dermatophytes | M. canis, T. verrucosum | Contact with infected pets (e.g., cats, dogs) or farm animals; more common in rural areas and among people who handle animals regularly |
| Geophilic dermatophytes | Microsporum species from soil | Contact with contaminated soil, often during gardening or farming; human-to-human spread is unusual |
| Host and environmental factors | - | Frequent animal contact, outdoor work with soil, crowding, and minor skin trauma increase the risk of infection |
Essential Investigations and Their Interpretation
Material for mycological investigation should be collected from the raised border of the lesion by scraping outwards with a blunt scalpel held perpendicular to the skin. If vesicles are present, the entire top should be submitted for examination.
Direct microscopic examination of infected material should reveal the branching hyphae characteristic of a dermatophyte infection.
Isolation of the aetiological agent in culture will allow the fungal species involved to be identified. This will provide information about the source of infection and help with selection of appropriate treatment.
In practice, microscopy provides rapid confirmation that a dermatophyte is present, whereas culture may take longer but helps distinguish between anthropophilic, zoophilic, and geophilic species. This distinction can be useful when advising patients about likely sources and when recognising possible outbreaks.
Management of Tinea Corporis
Topical antifungal preparations are the treatment of choice for localised lesions. Four imidazoles (clotrimazole, econazole, miconazole and sulconazole) and two allylamines (naftifine and terbinafine) are available in a number of topical formulations. All provide similarly high cure rates (70-100%), and adverse effects are uncommon. These medicines should be applied morning and evening for 2-4 weeks. Treatment should be continued for at least 1 week after the lesions have cleared, and the medicine should be applied at least 3 cm beyond the advancing margin of the lesion.
If the lesions are extensive or the patient does not respond to topical preparations, oral treatment is usually indicated. Itraconazole (100 mg/day for 2 weeks) and terbinafine (250 mg/day for 2-4 weeks) have proved more effective than griseofulvin (10 mg/kg per day for 4 weeks).
In addition to drug therapy, general measures such as keeping the skin dry, avoiding occlusive clothing, not sharing towels or sports equipment, and examining close contacts or household pets when appropriate can help reduce recurrence and transmission.
| Approach | When typically used | Examples mentioned | Duration from text |
|---|---|---|---|
| Topical imidazole therapy | Localised lesions; first-line treatment | Clotrimazole, econazole, miconazole, sulconazole | Applied morning and evening for 2-4 weeks, continued at least 1 week after clearance and at least 3 cm beyond lesion edge |
| Topical allylamine therapy | Localised lesions; alternative topical option | Naftifine, terbinafine | Applied morning and evening for 2-4 weeks, with similar extension beyond the advancing margin |
| Oral itraconazole | Extensive lesions or failure of topical therapy | Itraconazole 100 mg/day | 2 weeks |
| Oral terbinafine | Extensive lesions or failure of topical therapy | Terbinafine 250 mg/day | 2-4 weeks |
| Oral griseofulvin | Alternative systemic agent | Griseofulvin 10 mg/kg per day | 4 weeks |
| General measures | All patients, alongside antifungal therapy | Keeping skin dry, avoiding shared towels and equipment, assessing pets and close contacts | Throughout treatment and to prevent reinfection |

















