Diflucan (Fluconazole)

Dosages
Diflucan 50 mg
| Quantity | Price per tablet | Total price | |
|---|---|---|---|
| 60 | £0.70 | £42.23 | |
| 90 | £0.63 | £56.30 | |
| 120 | £0.59 | £70.38 | |
| 180 | £0.55 | £99.27 | |
| 270 | £0.53 | £142.97 | |
| 360 | £0.51 | £184.46 |
Diflucan 100 mg
| Quantity | Price per tablet | Total price | |
|---|---|---|---|
| 30 | £1.26 | £37.78 | |
| 60 | £0.95 | £57.04 | |
| 90 | £0.85 | £76.30 | |
| 120 | £0.80 | £95.56 | |
| 180 | £0.74 | £133.34 | |
| 270 | £0.71 | £190.39 |
Diflucan 150 mg
| Quantity | Price per tablet | Total price | |
|---|---|---|---|
| 30 | £1.61 | £48.15 | |
| 60 | £1.20 | £71.86 | |
| 90 | £1.06 | £95.56 | |
| 120 | £1.00 | £120.01 | |
| 180 | £0.93 | £167.42 | |
| 270 | £0.89 | £239.28 |
Diflucan 200 mg
| Quantity | Price per tablet | Total price | |
|---|---|---|---|
| 30 | £2.52 | £75.56 | |
| 60 | £1.83 | £109.64 | |
| 90 | £1.59 | £142.97 | |
| 120 | £1.48 | £177.05 | |
| 180 | £1.35 | £243.72 | |
| 270 | £1.28 | £345.95 |
Diflucan 400 mg
| Quantity | Price per tablet | Total price | |
|---|---|---|---|
| 30 | £4.20 | £125.94 | |
| 60 | £3.15 | £188.90 | |
| 90 | £2.81 | £252.61 | |
| 120 | £2.64 | £316.32 | |
| 180 | £2.46 | £443.00 | |
| 270 | £2.34 | £632.64 |
Payment & Delivery
Your order is carefully packed and is dispatched within 24 hours. Here is what a typical package looks like.
Sized like a regular personal letter (approximately 24x11x0.7 cm), with no indication of what is inside.



| Delivery Method | Estimated delivery |
|---|---|
| Express Free for orders over £222.24 | Estimated delivery to the UK: 4-7 days |
| Standard Free for orders over £148.16 | Estimated delivery to the UK: 14-21 days |










Discount Coupons
- New Year's Day - 1 January 2026 9% NEWYEAR9
- Valentine's Day - 14 February 2026 6% VALENTINE6
- St David's Day - 1 March 2026 4% DAVID4
- St Patrick's Day - 17 March 2026 5% PATRICK5
- St George's Day - 23 April 2026 4% GEORGE4
- May Day - 1 May 2026 5% MAYDAY5
- Halloween - 31 October 2026 6% HALLOWEEN6
- Guy Fawkes Night - 5 November 2026 5% GUY5
- Christmas Eve - 24 December 2026 9% XMASEVE9
- Christmas Day - 25 December 2026 10% XMAS10
- Boxing Day - 26 December 2026 10% BOXING10
- New Year's Eve - 31 December 2026 8% NYE8
Brand Names
| Country | Brand Names |
|---|---|
 Argentina Argentina | Candimicol Damicol Femixol Flucoginkan Fluconovag Fluzol Fungicil Fungocina Fungototal Honguil Plus Klonarizol Klonazol Micolis Novo Mutum Naxo C Nifurtox Niofen Periplum Ponaris Proseda F Triflucan |
 Australia Australia | Dizole Fluzole Ozole |
 Belgium Belgium | Candizole Fungimed |
 Brazil Brazil | Candix Candizol Celozol Farmazol Floltec Flucanil Flucanol Flucazol Flucocin Flucodan Flucoltrix Flucomed Fluconal Fluconax Fluconeo Fluconid Flucozen Flucozix Flunal Flunazol Fluotec Flusan Flutec Fungnon Glyflucan Helmicin Lertus Monipax Pantec Pronazol Riconazol Teczol Triazol Unizol Zelix Zolanix Zolmic Zolstatin Zoltec Zoltren |
 Czechia Czechia | Diflazon Fluco Forcan Mycomax Mycosyst Mykohexal |
 Denmark Denmark | Conasol Fungal |
 France France | Beagyne Triflucan |
 Germany Germany | Canex Canifug Fluco Fluc Flucobeta Flucoderm FlucoLich Flunazul Fungata |
 Greece Greece | Azoflu Azzol-S Dalrich Falipan Farviron Figalol Flucalit Flucocaps Flucodrug Flucofin Fluconapen Flucoran Flucozol Flukatril Flusenil Fluzomic Fumecal Funadel Fungo Fungram Fungustatin Fungusteril Fuxilidin Gynosant Hadlinol Medoflucon Mycazole Neomycol Opumyk Rifagen Stabilanol Tierlite Varmec Zidonil |
 Hungary Hungary | Dermyc Diflazon Flucohexal Flucoric Mycosyst Nofung |
 Italy Italy | Biozolene Elazor Flumicon Lefunzol Riflax Winch |
 Malaysia Malaysia | Avezol Biozole Flucon Fluconol Flucoric Flugal Fukole Medoflucon Odaft Stalene Zolstan |
 Mexico Mexico | Afungil Bioxel Candizol Difusel Fectrin Fharder Fleridux Flucoxan Fludisol Fluhexal Flukenol Flukezol Fluxes Fluxicap Fluzor Funser Lanfluzol Menifar Neofomiral Ongicil Oxifungol Ranflu Solarisol Terplex Waynazol Zilrin Zoldicam Zonal |
 Netherlands Netherlands | Flucoderm |
 New Zealand New Zealand | Canesten Fluconazole Flucazole |
 Poland Poland | Flucofast FlucoLEK Fluconazin Flumycon Mycomax Mycosyst |
 Portugal Portugal | Azoflune Fludocel Maxflin Reforce Supremase |
 Spain Spain | Citiges Lavisa Loitin Nesporac Solacap |
 Turkey Turkey | Biocanol Candidin Flucan Fluzole Fungan Kandizol Lumen Triflucan Trizol Zolax |
| Manufacturer | Brand Names |
|---|---|
| Cipla Limited | FCN Flucalup Forcan FZ |
| Inc. | FCN Flucalup Forcan FZ |
| Intas Pharmaceuticals Ltd. | FCN Flucalup Forcan FZ |
| Lupin Pharmaceuticals | FCN Flucalup Forcan FZ |
| Zenlabs Pharmaceutical Inc. | FCN Flucalup Forcan FZ |
FAQ
The health information contained herein is provided for educational purposes only. It is not intended to replace discussions with a healthcare professional. All decisions regarding patient care must be made by a healthcare professional, considering the unique characteristics of each patient.
The health information contained herein is provided for educational purposes only. It is not intended to replace discussions with a healthcare professional. All decisions regarding patient care must be made by a healthcare professional, considering the unique characteristics of each patient.
To find out more about Diflucan, please see our product information. No matter what type of treatment you use for a vaginal yeast infection, make sure to tell your doctor or other healthcare professional about any side effects you experience.
Diflucan is the only oral medication approved to treat yeast infections - it is 1 pill, 1 time. Diflucan has been proven to be as effective as 7 days of Monistat 7.
Description
Fluconazole is a widely used antifungal medicine that helps treat yeast and other fungal infections by stopping fungus from growing in the body. It comes in different strengths and is commonly prescribed when an effective, convenient oral treatment is needed. In the UK, it may be used in primary care or specialist settings when an oral antifungal is considered appropriate.
Uses
Before you buy Fluconazole online, read the important medicine information.
Fluconazole is used to treat oropharyngeal, oesophageal and vulvovaginal candidiasis, as well as other serious systemic candidal infections such as urinary tract infections, peritonitis, candidaemia, disseminated candidiasis, meningitis and pneumonia. It is also used to treat meningitis caused by Cryptococcus neoformans, as well as blastomycosis, coccidioidomycosis and histoplasmosis.

Fluconazole has also been used for less severe infections, including superficial fungal infections, dermatophytoses and onychomycosis. In addition, it is used to help prevent serious fungal infections such as coccidioidomycosis, cryptococcosis and mucocutaneous candidiasis in people with human immunodeficiency virus (HIV) infection, and to prevent fungal infections in other immunocompromised people, including cancer patients and bone marrow transplant recipients.
Before starting fluconazole treatment, suitable specimens for fungal culture and other relevant laboratory tests, such as serology and histopathology, should be obtained to isolate and identify the causative organism or organisms. Fluconazole may be started while these in vitro test results are pending; however, once the results are available, treatment should be adjusted accordingly. If fluconazole in vitro susceptibility tests are performed, the results should be interpreted with caution because the tests currently available may not accurately reflect fluconazole's in vivo activity.
Candidal Infections
Oropharyngeal and Oesophageal Candidiasis
Oral or IV fluconazole is used to treat oropharyngeal candidiasis in immunocompromised adults with acquired immunodeficiency syndrome (AIDS), advanced AIDS-related complex (ARC), malignancy or other severe underlying disease. It is also used orally or by IV infusion to treat oesophageal candidiasis in adults with AIDS, malignancy or other severe underlying disease, including progressive systemic sclerosis.
Fluconazole appears to be at least as effective as, and in some cases more effective than, other antifungal agents used for the initial treatment of oropharyngeal and/or oesophageal candidal infections. It is considered a drug of choice for these infections.
Fluconazole has produced clinical resolution of signs and symptoms of infection in 79-100% of patients with oropharyngeal candidiasis; however, microbiological cures have generally been obtained in 44-87% of patients, and the relapse rate may be high, especially in neutropenic patients. In adults with oesophageal candidiasis confirmed by endoscopy, fluconazole has produced clinical resolution of signs and symptoms of infection in about 61-93% of patients. In one study in adults with oesophageal candidiasis and progressive systemic sclerosis, fluconazole treatment produced mycological cures in about 93% of patients within 2-4 weeks. However, the relapse rate was almost 100% within 3 months after fluconazole was stopped.
Patients with HIV infection who have severe or recurrent episodes of oropharyngeal or oesophageal candidiasis may benefit from long-term suppressive or maintenance treatment to help prevent relapse.
Some clinicians consider topical treatment with oral clotrimazole or oral nystatin to be the treatment of choice for uncomplicated oropharyngeal candidiasis in people with HIV infection, and recommend that systemic antifungal agents such as oral fluconazole, oral itraconazole or oral ketoconazole should be reserved for oropharyngeal candidiasis that does not respond to topical treatment and for severe oropharyngeal candidiasis with oesophageal involvement. However, some clinicians prefer to use an oral azole antifungal for initial treatment of oropharyngeal candidiasis.
Oral fluconazole or itraconazole oral solution is at least as effective as topical treatment. In a study of adults with HIV infection and oropharyngeal candidiasis, the response rate and mycological eradication rate after 14 days of treatment were 100 and 75%, respectively, in those who received oral fluconazole (100 mg once daily), compared with 65 and 20%, respectively, in those who received topical clotrimazole (10-mg oral lozenge 5 times daily). In another study, 14 days of treatment with oral fluconazole (100 mg once daily as an oral suspension) was more effective than 14 days of topical nystatin (500,000 units as an oral suspension 4 times daily). The mycological cure rate was 60% in the fluconazole group and 6% in the nystatin group, and the relapse rate at day 42 was 27 and 11%, respectively. After long-term follow-up, the comparative effectiveness of fluconazole and other antifungal agents needs further study.
Systemic anti-infective treatment is necessary for oesophageal candidiasis. Some clinicians state that a 14- to 21-day course of oral fluconazole (100 mg once daily) or itraconazole oral solution (200 mg once daily) is highly effective for treating oesophageal candidiasis, and that oral ketoconazole is less effective. These clinicians suggest that an oral itraconazole solution should be used in patients who do not respond to oral fluconazole. IV amphotericin B can be used in patients with otherwise refractory disease. In a randomised, multicentre, double-blind study comparing oral fluconazole (initial dosage 100 mg daily increased to 200 mg daily if no symptomatic improvement occurred within 1-2 weeks) for up to 8 weeks with oral ketoconazole (initial dosage 200 mg daily increased to 400 mg daily if no symptomatic improvement occurred within 1-2 weeks) in patients with AIDS and endoscopically confirmed oesophageal candidiasis, endoscopic cure and resolution of oesophageal symptoms occurred in 91 and 85% of patients receiving fluconazole, respectively, while endoscopic cure and resolution of symptoms occurred in 52 and 65% of patients receiving ketoconazole, respectively. Results of another study in immunocompromised patients with oesophageal candidiasis indicate that patients receiving fluconazole may require a shorter duration of initial treatment than those receiving ketoconazole.
Vulvovaginal Candidiasis
Oral fluconazole is used to treat uncomplicated vulvovaginal candidiasis and complicated vulvovaginal candidiasis in non-pregnant women. Before antifungal treatment is first used in a woman with signs and symptoms of uncomplicated vulvovaginal candidiasis, the diagnosis should be confirmed either by showing yeasts or pseudohyphae on direct microscopic examination of vaginal discharge (10% potassium hydroxide [KOH] wet mount or Gram stain) or by culture. Identifying Candida by culture in the absence of symptoms is not an indication for antifungal treatment, since around 10-20% of women carry Candida or other yeasts in the vagina. In women with recurrent vulvovaginal candidiasis, vaginal cultures should be taken to confirm the diagnosis and identify unusual Candida species such as C. glabrata.
Uncomplicated Vulvovaginal Candidiasis
Oral fluconazole effectively treats uncomplicated vulvovaginal candidiasis when given as a single dose. A single 150-mg oral dose of fluconazole produces clinical cures, meaning the absence of vulvovaginal burning, itching, swelling, erythema, excoriation, dyspareunia and/or ulceration together with a substantial reduction in vaginal discharge, 5-16 days after the dose in around 90-100% of non-pregnant women with uncomplicated vulvovaginal candidiasis. Mycological cures occur in around 77-100%. At 27-62 days after the single dose, clinical and mycological cure rates are 61-90%, and the rate of relapse, reinfection or recolonisation is about 23%. Results of several studies in patients with uncomplicated vulvovaginal candidiasis suggest that a single 150-mg dose of oral fluconazole is as effective for this condition as multiple-dose regimens of intravaginal clotrimazole, econazole, miconazole or terconazole. In addition, the single-dose oral fluconazole regimen is as effective for uncomplicated vulvovaginal candidiasis as oral itraconazole or oral ketoconazole.
In controlled studies in patients with vulvovaginal candidiasis, clinical and mycological cure rates at 14 and 30-35 days were similar in patients receiving oral fluconazole (given as a single 150-mg dose) and in patients receiving intravaginal clotrimazole (given as a 100-mg vaginal tablet once daily for 7 days) or miconazole (given as a 100-mg vaginal cream once daily for 7 days). At 14 days, the clinical cure rate was reported to be about 95-96% with fluconazole and 95-97% with intravaginal clotrimazole or miconazole, and the mycological cure rate was reported to be 77-80% with fluconazole and 72-82% with intravaginal clotrimazole or miconazole. At 30-35 days, the clinical cure rate was reported to be about 69-75% with fluconazole and 72-80% with intravaginal clotrimazole or miconazole, and the mycological cure rate was reported to be 61-63% with fluconazole and 57-63% with intravaginal clotrimazole or miconazole.
UK clinical guidance and other clinicians recommend that uncomplicated vulvovaginal candidiasis, defined as vulvovaginal candidiasis that is mild to moderate, sporadic or infrequent, most likely caused by C. albicans, or occurring in immunocompetent women, should be treated with an intravaginal azole antifungal such as butoconazole, clotrimazole, miconazole, terconazole or tioconazole, given as an appropriate single-dose or short-course regimen, or with a single oral dose of fluconazole. These regimens have generally been associated with clinical and mycological cure rates of 80-90% in otherwise healthy, non-pregnant women with uncomplicated infections. Some clinicians suggest that a single oral dose of fluconazole may offer an advantage over conventional intravaginal treatment because it helps support adherence and may reduce or eliminate concurrent rectal infection that can act as a source of reinfection. When weighing up the potential risks and benefits of oral versus intravaginal treatment, the potential for toxicity such as hepatotoxicity and for drug interactions with oral treatment should be considered. Side effects are more common in patients receiving a single oral dose of fluconazole than in those receiving intravaginal treatment, and this should also be considered carefully.
Complicated and Recurrent Vulvovaginal Candidiasis
Oral fluconazole is used to treat complicated vulvovaginal candidiasis, including recurrent and severe infections. Complicated vulvovaginal candidiasis is defined as infections that are recurrent or severe, caused by Candida species other than C. albicans, or occurring in pregnant women or women with underlying conditions such as uncontrolled diabetes, debilitation or immunosuppression.
Optimum regimens for treating recurrent vulvovaginal candidiasis, usually defined as 4 or more episodes of symptomatic vulvovaginal candidiasis each year, have not been established. Although each episode caused by C. albicans may respond to the usual single-dose oral fluconazole or short-course intravaginal antifungal treatment, a longer initial course may be needed to achieve mycological remission, and long-term maintenance treatment may be required to prevent relapse. UK guidance and other clinicians recommend an initial intensive regimen of 7-14 days of an intravaginal azole antifungal or a 2-dose regimen of oral fluconazole (150 mg repeated 3 days later), followed by a maintenance antifungal regimen for 6 months. For maintenance treatment, regimens such as intravaginal clotrimazole (500 mg once weekly), oral ketoconazole (100 mg once daily), oral fluconazole (100 mg-150 mg once weekly), or oral itraconazole (400 mg once monthly or 100 mg once daily) have been used. These maintenance regimens can effectively reduce recurrent infections; however, 30-40% of women will have recurrent disease once maintenance treatment is stopped.
The response rate to short-course antifungal regimens is lower in patients with severe vulvovaginal candidiasis, meaning extensive vulval erythema, oedema, excoriation and fissure formation. Either a 2-dose regimen of oral fluconazole (150 mg repeated 3 days later) or 7-14 days of an intravaginal azole antifungal is recommended for these infections. These longer regimens may also be necessary for the treatment of vulvovaginal candidiasis in women with underlying debilitating medical conditions, such as uncontrolled diabetes or corticosteroid treatment. Vulvovaginal candidiasis may occur more often and may be more severe in women with human immunodeficiency virus (HIV) infection than in women without HIV infection. These infections have been recognised as an early manifestation of acquired immunodeficiency syndrome (AIDS) in women. While the optimum treatment for recurrent vulvovaginal candidiasis in women with HIV infection has not been established, there is no evidence to date that these women have a lower response rate to the intravaginal or oral antifungal regimens usually recommended for vulvovaginal candidiasis. Therefore, UK clinical guidance and other clinicians advise that treatment of vulvovaginal candidiasis in women with HIV infection should be the same as that in women without HIV infection.
Recurrent vulvovaginal candidiasis may rarely be caused by resistant strains of C. albicans or, more commonly, by other Candida species with reduced susceptibility to azole antifungal agents such as C. glabrata. It has been suggested that repeated treatment of recurrent vulvovaginal candidiasis with intravaginal azole antifungal agents, together with widespread and/or inappropriate self-treatment, may favour the selection of Candida species that are resistant to azole antifungal agents. Optimum treatment for vulvovaginal candidiasis caused by Candida with reduced susceptibility to azole antifungal agents has not been established. For vulvovaginal candidiasis caused by Candida species other than C. albicans, UK clinical guidance generally advises 7-14 days of treatment with an antifungal agent other than fluconazole; if recurrence occurs, intravaginal boric acid (600-mg capsule once daily for 2 weeks) may be used. Referral to a specialist is advised.
Candidaemia and Other Candidal Infections
Fluconazole has effectively treated serious candidal urinary tract infections, peritonitis and pneumonia. It has also been effective in the treatment of chronic mucocutaneous candidiasis, candidaemia, chronic disseminated candidiasis (hepatosplenic candidiasis), candidal endocarditis, candidal meningitis, candidal osteomyelitis and other severe systemic candidal infections. It has been effective in treating some candidal infections that did not respond to amphotericin B. Fluconazole has also been effective in treating life-threatening candidal infections in organ transplant patients receiving immunosuppressive treatment. In some renal allograft recipients, fluconazole treatment effectively eliminated fungal infections without stopping or reducing the dosage of immunosuppressive treatment.
Both IV amphotericin B and IV or oral fluconazole are considered drugs of choice for systemic invasive candidiasis; however, the best antifungal regimens for these infections have been difficult to identify, and each medicine has drawbacks. While fluconazole may be better tolerated and easier to give than IV amphotericin B, fluconazole-resistant strains of C. albicans are being isolated more often from patients who have previously received fluconazole, especially patients with HIV infection. Some candidal infections, such as candidaemia, are increasingly caused by strains that are intrinsically resistant to fluconazole, such as C. krusei, or are likely to be fluconazole-resistant, such as C. glabrata. The choice of antifungal agent for the initial treatment of invasive candidal infections should take into account local and/or institutional epidemiological data on the prevalence of the various candidal strains and their resistance patterns, the patient's colonisation status, the severity and duration of neutropenia or immunosuppression, and any history of prior fluconazole use. Most clinicians recommend IV amphotericin B if the infecting organism is known or likely to be C. krusei; however, fluconazole is preferred if C. lusitaniae causes the infection.
Because candidaemia is associated with substantial morbidity and a risk of long-term sequelae, antifungal treatment is generally recommended for all patients with candidaemia, whether neutropenic or non-neutropenic, in addition to removal and/or replacement of any intravascular catheters. It has been suggested that oral fluconazole may be preferred over IV amphotericin B for treating candidaemia in non-neutropenic patients, whether stable or unstable, unless there is evidence that the infection is caused by fluconazole-resistant strains or the patient has previously received fluconazole. IV amphotericin B is generally preferred for severe candidaemia in patients whose infections may be caused by fluconazole-resistant strains such as C. krusei or C. glabrata, in patients who have recently received fluconazole, and in immunocompromised patients such as those with HIV infection. In a controlled study in patients with candidaemia who were immunocompetent and had normal neutrophil counts, the response to conventional IV amphotericin B therapy ( mg/kg daily for 7 days, then 3 times weekly for an additional 10 days) or fluconazole therapy (400 mg daily given IV for 7 days, then orally for an additional 11 days) was similar. Both regimens appeared to be equally effective. The overall response rate to a conventional IV amphotericin B regimen or oral fluconazole was also similar in a prospective, randomised study that included non-neutropenic and neutropenic patients with documented or presumed invasive candidiasis. However, further study is needed to more fully evaluate the relative effectiveness of amphotericin B and fluconazole in immunocompromised patients or patients with severe infections.
Oral fluconazole or IV amphotericin B are recommended when treatment of candiduria is indicated, for example in symptomatic or neutropenic patients, low-birthweight infants, patients with renal allografts, or patients who will undergo urological procedures. Fluconazole may be preferred unless C. krusei or C. glabrata causes the infection. Bladder irrigation with conventional amphotericin B has also been used. In a randomised study in hospitalised geriatric patients with fungi caused by C. albicans, C. tropicalis or C. glabrata, 5 days of bladder irrigation with conventional amphotericin B (25 mg of amphotericin B in 500 mL of 5% dextrose injection infused through an indwelling bladder catheter at a rate of 42 mL/hour) or a 5-day course of oral fluconazole (200-mg loading dose on day 1 followed by 100 mg once daily for four additional days) eradicated the funguria in 83 or 66% of patients, respectively.
Fluconazole is also used prophylactically to reduce the incidence of candidiasis in bone marrow transplant recipients who are receiving chemotherapy or radiotherapy. It has also been used for primary prophylaxis against fungal infections, including candidiasis, in a limited number of patients considered to be at high risk of developing such infections, such as neutropenic cancer patients, those colonised with Candida and/or receiving corticosteroids, and certain patients with AIDS.
Fluconazole has been used with good results in several patients with endophthalmitis caused by Candida. However, treatment failures have also been reported, and the role of the medicine in treating this infection remains unclear. Studies in rabbits indicate that fluconazole is distributed into the eye and that it inhibits the growth of C. albicans in rabbit choroid-retina tissue and vitreous body when IV treatment is started within 24 hours after inoculation; it did not effectively inhibit growth of the organism when IV treatment was started 7 days after inoculation, when the infection was well established.
Cryptococcal Infections
Oral or IV fluconazole is used in immunocompetent or immunocompromised adults to treat meningitis caused by C. neoformans. It has been effective for the initial treatment of acute cryptococcal meningitis in both adults with HIV infection and HIV-negative adults. It has produced clinical resolution of signs and symptoms of infection in approximately 34-75% of these patients. Although amphotericin B, with or without concomitant flucytosine, has been considered the initial treatment of choice for cryptococcal meningitis, fluconazole is an alternative for patients whose disease is not severe because it is generally well tolerated and reaches high concentrations in cerebrospinal fluid (CSF). While experience in children is limited, fluconazole may also be considered as an alternative to amphotericin B in this age group.
Fluconazole has been effective in treating acute cryptococcal meningitis in some patients who did not respond to amphotericin B. However, some evidence suggests that fluconazole may be less effective than amphotericin B in the early treatment of acute cryptococcal meningitis in patients with AIDS and may clear the infection from the CSF more slowly. In a randomised multicentre study comparing amphotericin B (mean dosage of 0.4-0.5 mg/kg daily for 10 weeks, with or without flucytosine) with oral fluconazole (400 mg on the first day and 200-400 mg thereafter for 10 weeks) in AIDS patients with cryptococcal meningitis, treatment was effective in 40% of patients receiving amphotericin B and in 34% of those receiving fluconazole. Although overall mortality was similar in the two groups (14% with amphotericin B versus 18% with fluconazole), mortality during the first 2 weeks of treatment was higher in patients receiving fluconazole (15% versus 8% with amphotericin B). CSF cultures remained positive for an average of about 42 days in patients receiving amphotericin B and 64 days in those receiving fluconazole. In another study comparing amphotericin B (0.7 mg/kg daily for 1 week, followed by the same dose 3 times weekly for 9 weeks combined with flucytosine 150 mg/kg daily) with oral fluconazole (400 mg daily for 10 weeks) in a limited number of AIDS patients with cryptococcal meningitis, initial treatment was effective in all patients receiving amphotericin B but in only 43% of those receiving fluconazole; CSF cultures were positive for an average of about 16 and 41 days in patients receiving these respective treatments. While the patient groups in this study were similar in terms of the severity of cryptococcal infection, the helper/inducer (CD4+, T4+) T-cell count was lower in the fluconazole group, which makes interpretation more difficult.
Many clinicians recommend starting treatment of cryptococcal meningitis in HIV-infected patients with IV amphotericin B (with flucytosine) for at least 2 weeks, or until the patient's condition has stabilised, followed by oral fluconazole or oral itraconazole for at least another 8-10 weeks or longer. Pending more data and clinical experience, some clinicians consider it most prudent to use initial (primary) treatment with IV amphotericin B, with or without flucytosine, followed by fluconazole maintenance therapy, at least in patients with more severe disease and those at high risk. They suggest that primary fluconazole therapy should probably be reserved for patients who do not respond adequately to amphotericin B, cannot tolerate it, or have less severe disease (for example, no neurological symptoms and low CSF cryptococcal antigen titres).
The relative efficacy of initial treatment with conventional IV amphotericin B given with flucytosine (100 mg/kg daily) or placebo for 2 weeks, followed by oral fluconazole (800 mg daily for 2 days, then 400 mg daily for 8 weeks) or oral itraconazole (600 mg daily for 3 days, then 400 mg daily for 8 weeks), has been evaluated in a double-blind multicentre trial in patients with AIDS-associated cryptococcal meningitis. At 2 weeks, CSF cultures were negative in 60% of those who received amphotericin B with flucytosine compared with 51% of those who received amphotericin B alone. The clinical response to oral fluconazole or oral itraconazole as follow-up treatment was similar. However, the rate of CSF sterilisation at 10 weeks was higher in those who received fluconazole (72%) than in those who received itraconazole (60%).
A regimen of oral fluconazole (400 mg daily for pulmonary infections or 400-800 mg daily for CNS infections) and oral flucytosine (100-150 mg/kg daily) has been used as an alternative treatment for pulmonary or CNS cryptococcal infections in a limited number of patients. Although fluconazole used with flucytosine may be effective for mild to moderate pulmonary cryptococcal infections, this regimen has been ineffective in some patients with cryptococcal meningitis. It is not recommended as initial treatment for these infections. In addition, when used to treat cryptococcal meningitis in HIV-infected people, a regimen of fluconazole and flucytosine has been associated with a high rate of side effects, leading to discontinuation of flucytosine in 28% of patients.
The mortality rate in AIDS patients during the first episode of cryptococcal meningitis has been about 25-58% despite amphotericin B treatment. In patients with AIDS who respond to initial antifungal treatment, the relapse rate for cryptococcal infection is 35-65%. Long-term maintenance or suppressive antifungal treatment is generally considered necessary after initial treatment of the infection unless immune recovery has occurred with effective antiretroviral therapy.
Oral fluconazole has been effective as long-term maintenance treatment to prevent relapse of cryptococcal meningitis in patients with AIDS. (See Uses: Prevention of Fungal Infections in HIV-infected Individuals.) Results of a multicentre study comparing the safety and efficacy of oral fluconazole (200 mg once daily) with IV amphotericin B (1 mg/kg once weekly) for preventing relapse in AIDS patients who had negative cryptococcal cultures after adequate initial amphotericin B treatment indicate that the fluconazole regimen is more effective, in terms of preventing relapse of culture-positive meningitis, and better tolerated than amphotericin B for maintenance treatment in these patients. In a multicentre study comparing oral fluconazole maintenance (100-200 mg daily) with placebo in such patients, the overall calculated cumulative risk of cryptococcal recurrence at any site after 1 year of fluconazole maintenance was 5% versus 100% for placebo.
The effectiveness of fluconazole maintenance in preventing cryptococcal relapse in patients with persistent prostatic infection after primary antifungal treatment appears to be lower than in patients overall. Still, this reduced effect may be at least partly overcome by increasing the dosage. In a limited number of adults with AIDS who had persistent urinary cryptococcosis, including prostate infections, after adequate primary amphotericin B treatment with or without flucytosine for cryptococcal meningitis, oral fluconazole maintenance therapy resulted in mycological cures in most patients. In contrast, relapse of cryptococcosis (with prostatic massage) and/or systemic infection occurred in the remaining patients during fluconazole maintenance.
Response, defined as sustained suppression of prostatic massage-induced cryptococcus and no evidence of systemic or CNS relapse, appears to be dose-dependent in these patients and generally requires oral fluconazole 200-600 mg daily. It also takes several weeks to months of fluconazole maintenance before this becomes apparent; in one study, the probability of response was estimated to be 36% after 4 weeks and 59% after 27 weeks of maintenance. Relatively large dosages (for example, 600 mg or more daily) may effectively sterilise multiple large prostatic abscesses in some patients. However, the factors that may predict response and the best antifungal treatment in these patients still need to be defined more clearly. In addition, because of the risk of relapse, some clinicians caution that a prostatic focus of infection should be carefully ruled out in any male patient if low-dose fluconazole maintenance is being considered.
Oral fluconazole has been effective in a limited number of patients for treating cutaneous or subcutaneous cryptococcosis. The drug has also been effective in treating cryptococcal pneumonia in a limited number of patients, although surgical removal of the focus of infection was necessary in some cases. However, the possibility that cryptococcal pneumonia may be a sign of disseminated infection should be considered.
Coccidioidomycosis
Oral fluconazole has been used successfully to treat coccidioidomycosis caused by Coccidioides immitis (for example, meningitis, pulmonary infections, and disseminated infections including soft tissue or bone and joint involvement). In adults with coccidioidal meningitis, fluconazole has produced clinical and/or laboratory signs of improvement when used alone or together with amphotericin B treatment. Oral fluconazole has been used to treat coccidioidal meningitis in both HIV-infected and HIV-negative individuals. Because fluconazole is generally well tolerated and has favourable pharmacokinetics (for example, it reaches high concentrations in the CSF after oral or IV administration), it is considered a less toxic alternative to amphotericin B for coccidioidal meningitis and other persistent coccidioidal infections, especially as long-term antifungal treatment is usually needed for these infections. Fluconazole is considered a drug of choice for treating coccidioidomycosis; however, IV amphotericin B is generally preferred as the initial treatment for severe coccidioidomycosis, especially in immunocompromised patients, including people with HIV. More study is needed to assess how effective fluconazole is, establish the optimum oral dosage for coccidioidomycosis, and determine whether it substantially reduces morbidity and mortality. Some data suggest that response rates may improve when higher fluconazole dosages (that is, 400 mg daily or higher) are used. It has been suggested that relatively low dosages (for example, 50-100 mg daily) may contribute to the risk of recurrence.
Blastomycosis
Oral fluconazole has been used to treat North American blastomycosis caused by Blastomyces dermatitidis. While oral itraconazole or IV amphotericin B are considered drugs of choice for blastomycosis, oral fluconazole or oral ketoconazole are considered alternatives. IV amphotericin B is generally preferred for severe infections, especially those involving the CNS, and for the initial treatment of presumed blastomycosis in immunocompromised patients, including people with HIV.
There is some evidence that oral itraconazole may be more effective than oral fluconazole or oral ketoconazole for blastomycosis. Many clinicians consider itraconazole the preferred azole antifungal for non-meningeal, non-life-threatening blastomycosis and also recommend it as follow-up treatment in patients with more severe infections after an initial response to IV amphotericin B. When choosing an antifungal for patients with blastomycosis, it should be remembered that treatment failures have been reported when an oral antifungal (for example, ketoconazole) was used for cutaneous or pulmonary blastomycosis in patients who had asymptomatic or subclinical CNS involvement at the time of the initial diagnosis.
Histoplasmosis
Oral fluconazole has been used with some success to treat histoplasmosis caused by Histoplasma capsulatum. While IV amphotericin B or oral itraconazole are considered drugs of choice for histoplasmosis, oral fluconazole or oral ketoconazole are considered alternatives. Oral fluconazole (400-800 mg daily) has been effective in a limited number of HIV-infected patients with mild or moderately severe disseminated histoplasmosis. However, IV amphotericin B is generally preferred for the initial treatment of severe, life-threatening histoplasmosis, especially in immunocompromised patients such as those with HIV infection. In addition, oral itraconazole is generally the preferred azole antifungal for treating mild to moderate histoplasmosis or as follow-up treatment for severe infections after a response has been achieved with amphotericin B.
Sporotrichosis
Fluconazole is used as an alternative treatment for sporotrichosis. IV amphotericin B is usually considered the treatment of choice for the initial management of severe, life-threatening infections and whenever there is CNS involvement, while oral itraconazole is considered the treatment of choice for cutaneous, lymphocutaneous, or mild pulmonary or osteoarticular sporotrichosis and for follow-up treatment in more severe infections after a response has been achieved with IV amphotericin B. Fluconazole is considered second-line treatment for cutaneous, lymphocutaneous, or osteoarticular sporotrichosis and, because it may be less effective than itraconazole, should be used only if the patient cannot tolerate itraconazole. Some clinicians state that fluconazole is not effective and should not be used to treat pulmonary sporotrichosis.
Aspergillosis
Fluconazole has been used orally, by IV infusion, or by intracavitary infusion in a few adults to treat pneumonia or other respiratory tract infections caused by Aspergillus fumigatus, A. niger, or A. terreus. In one study, fluconazole had a clinical efficacy rate of 23-53% in Aspergillus infections and a mycological cure rate of about 50% for A. fumigatus infections. Fluconazole has produced variable results in the treatment of Aspergillus infections. IV amphotericin B is generally considered the treatment of choice, and itraconazole is usually the preferred alternative for aspergillosis.
Dermatophytoses
Oral fluconazole has been effective in the treatment of certain dermatophyte infections (for example, tinea capitis, tinea corporis, tinea cruris, and tinea pedis) caused by Epidermophyton, Microsporum, or Trichophyton. Oral fluconazole has also been effective for treating pityriasis (tinea) versicolor and onychomycosis.
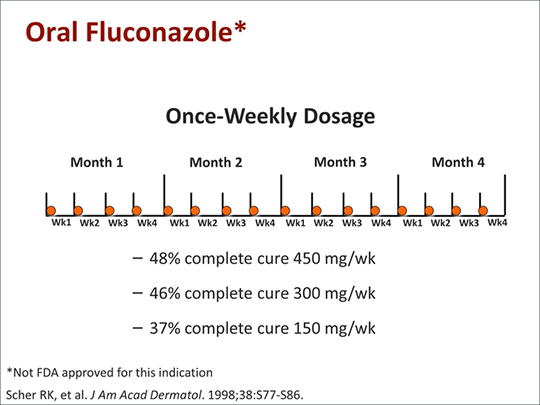
Oral fluconazole (3-6 mg/kg daily for 2-6 weeks) has effectively treated tinea capitis in children aged 1.5-16 years and has resulted in clinical and mycological cure in about 88-90% of patients. For tinea corporis, tinea cruris, or tinea pedis in adults, oral fluconazole has been effective as a once-weekly regimen (150 mg once weekly for 2-6 weeks). There is evidence that this once-weekly regimen is as effective as a once-daily regimen of the drug (50 mg once daily) for these infections. Results of a randomised study indicate that the eradication rate at the end of treatment in patients with tinea corporis or tinea cruris is 82-88% in those receiving the once-weekly regimen and 94-100% in those receiving the once-daily regimen; at 1-month follow-up, the overall eradication rates were 91-100 or 91-94%, respectively. Although the optimum oral fluconazole dosage regimen for onychomycosis has not been established, a once-weekly oral fluconazole regimen (150-450 mg once weekly for 3-12 months) has been effective for toenail onychomycosis in a limited number of adults. However, more study is needed, and there is some evidence that fluconazole may be less effective than oral itraconazole or oral terbinafine for treating onychomycosis.
Tinea corporis and tinea cruris can usually be treated effectively with a topical antifungal. However, an oral antifungal may be needed if the disease is extensive, dermatophyte folliculitis is present, the infection is chronic or does not respond to topical treatment, or the patient is immunocompromised or has coexisting disease. Tinea capitis and tinea barbae are generally treated with an oral antifungal. While topical antifungals are usually adequate for uncomplicated tinea manuum and tinea pedis, an oral antifungal is usually needed for hyperkeratotic areas of the palms and soles, chronic moccasin-type (dry-type) tinea pedis, and tinea unguium (onychomycosis).
Prevention of Fungal Infections in HIV-infected Individuals
Fluconazole has been used in HIV-infected individuals for primary prophylaxis against serious fungal infections (for example, cryptococcosis) and for long-term suppressive or maintenance therapy (secondary prophylaxis) to prevent recurrence or relapse of certain fungal infections (for example, coccidioidomycosis, cryptococcosis, and mucocutaneous candidiasis).
In the UK, guidance on preventing opportunistic infections, including fungal infections, in people with HIV covers prevention of exposure to opportunistic pathogens, prevention of first disease episodes, and prevention of disease recurrence. UK guidance does not recommend primary prophylaxis to prevent first episodes of mucocutaneous candidiasis in adults, adolescents, infants, and children with HIV infection. While routine primary prophylaxis to prevent first episodes of coccidioidomycosis, cryptococcosis, or histoplasmosis is also not generally recommended, prophylaxis against cryptococcosis or histoplasmosis may be considered in selected individuals. UK guidance also supports long-term suppressive or maintenance therapy (secondary prophylaxis) after initial treatment for documented coccidioidomycosis, cryptococcosis, or histoplasmosis to help prevent recurrence or relapse. In addition, people with HIV infection who have frequent or severe recurrences of mucocutaneous candidiasis (oropharyngeal, oesophageal, vaginal) may benefit from long-term suppressive or maintenance therapy.
Because of concerns about the use of oral azole antifungals during pregnancy, fluconazole should not be used for primary prophylaxis or long-term suppressive or maintenance therapy in pregnant women. If a woman becomes pregnant while receiving fluconazole prophylaxis and chooses to continue the pregnancy, prophylaxis should be stopped. Effective contraception is recommended for all HIV-infected women receiving an oral azole antifungal for suppressive therapy. Conventional IV amphotericin B may be the preferred option if long-term suppressive or maintenance therapy against coccidioidomycosis, cryptococcosis, or histoplasmosis is needed in an HIV-infected pregnant woman, especially during the first trimester.
Primary Prophylaxis
Coccidioidomycosis
In UK practice, routine primary prophylaxis against coccidioidomycosis is not generally recommended for people with HIV. Some clinicians may consider prophylaxis for those with positive CF serology in the absence of active disease, but it remains unclear whether this is beneficial. Cases of active coccidioidomycosis have occurred in people with HIV who were already receiving azole therapy for other conditions. Routine skin testing is not generally recommended and does not reliably predict disease, and routine serological testing is also not usually considered helpful, although a positive serological result may indicate increased risk in someone with relevant exposure.
Cryptococcosis
In UK practice, routine primary prophylaxis against cryptococcosis is not generally recommended, although it may be considered in adults and adolescents with HIV whose CD4+ T-cell counts are below 50/mm3 and in infants and children with severe immunosuppression, as defined by age-adjusted criteria. Routine prophylaxis is not advised because cryptococcal disease is relatively uncommon, there is no clear evidence of a survival benefit, and there are concerns about drug interactions, the potential for resistance, and cost. The need for primary prophylaxis or suppressive therapy against other fungal infections, such as coccidioidomycosis, histoplasmosis, or mucocutaneous candidiasis, should also be taken into account when considering prophylaxis against cryptococcosis. Routine serum cryptococcal antigen testing in asymptomatic people is not generally recommended because the result is unlikely to alter management. People with HIV cannot completely avoid exposure to Cryptococcus neoformans, and there is no evidence that exposure to pigeon droppings increases the risk of cryptococcosis.
Oral fluconazole is the treatment of choice for primary prophylaxis against cryptococcosis in HIV-infected adults, adolescents, infants, and children, and itraconazole (given as oral capsules) is considered an alternative.
Histoplasmosis
In UK practice, primary prophylaxis against histoplasmosis may be considered for adults or adolescents with HIV whose CD4+ T-cell counts are below 100/mm3 if they are at particularly high risk of exposure to Histoplasma capsulatum, for example through occupational exposure, or if they have lived in a community with a very high burden of histoplasmosis. It may also be considered for infants or children with HIV who have severe immunosuppression and relevant exposure risk. When deciding whether to use primary prophylaxis in these patients, clinicians should take into account the likely local incidence of histoplasmosis, the possibility of drug interactions, toxicity, the risk of resistance, cost, and whether prophylaxis is also needed against other fungal infections such as candidiasis or cryptococcosis.
The first-choice agent for primary prophylaxis against histoplasmosis in HIV-infected adults, adolescents, or paediatric patients is oral itraconazole (given as capsules); the USPHS/IDSA makes no recommendation regarding an alternative to itraconazole. There is some evidence that oral fluconazole may be ineffective in preventing first episodes of histoplasmosis.
Mucocutaneous Candidiasis
The USPHS/IDSA states that primary prophylaxis to prevent first episodes of mucocutaneous candidiasis (oesophageal, oropharyngeal, vaginal) in HIV-infected adults, adolescents, infants, or children is not recommended because acute mucocutaneous candidiasis is generally treatable and rarely life-threatening and because of concerns about the potential for resistant Candida to develop, the possibility of drug interactions, and the cost of antifungal prophylaxis.
Prevention of Recurrence
Coccidioidomycosis
In UK practice, people with HIV who have completed initial treatment for documented coccidioidomycosis should usually receive long-term suppressive or maintenance therapy to reduce the risk of recurrence or relapse. Oral fluconazole is generally the preferred option, with IV amphotericin B and oral itraconazole capsules as alternatives. In adults, adolescents, infants and children with HIV, suppressive therapy is often continued for life. Although the risk of recurrent systemic fungal infection may be lower in those whose CD4+ T-cell count rises above 100/mm3 on effective combination antiretroviral therapy, current evidence is still not enough to make a clear recommendation on stopping prophylaxis against coccidioidomycosis.
Cryptococcosis
In UK practice, people with HIV who have completed initial treatment for documented cryptococcosis should usually receive long-term suppressive or maintenance therapy to prevent recurrence or relapse unless immune recovery has occurred with effective combination antiretroviral therapy. Oral fluconazole is generally the preferred option, with IV amphotericin B and oral itraconazole capsules as alternatives. Evidence from a randomised, double-blind, controlled study in people with HIV and adequately treated cryptococcal meningitis suggests that oral fluconazole 200 mg once daily is more effective than oral itraconazole 200 mg once daily for suppressive therapy, with culture-positive relapse rates of 4% and 23% respectively.

Suppressive or maintenance therapy to prevent recurrence or relapse of cryptococcosis in people with HIV is generally continued for life unless immune recovery has occurred as a result of effective combination antiretroviral therapy. Limited data suggest that stopping suppressive or maintenance therapy in adults and adolescents with HIV who have completed initial therapy for cryptococcosis, remain free of symptoms related to cryptococcosis, and have sustained increases in CD4+ T-cell counts to greater than 100-200/mm3 for 6 months or longer in response to effective antiretroviral therapy is associated with a low risk of recurrence. Based on this and more extensive cumulative data on the safety of stopping long-term suppressive therapy for other opportunistic infections, the USPHS/IDSA states that it is reasonable to consider discontinuing suppressive therapy in people who meet these criteria. The USPHS/IDSA notes that recurrences could occur in people who stop suppressive therapy and states that suppressive therapy should be restarted if the CD4+ T-cell count falls to less than 100-200/mm3. The safety of stopping suppressive therapy in infants and children with HIV has not been studied, and children should receive lifelong suppressive therapy after an episode of cryptococcosis.
Histoplasmosis
For long-term suppressive therapy in patients with HIV and documented histoplasmosis that has been adequately treated, the USPHS/IDSA states that oral itraconazole capsules are the treatment of choice and IV amphotericin B is an alternative.
Mucocutaneous Candidiasis
In UK practice, long-term suppressive or maintenance therapy should be considered for adults and adolescents with a history of documented oesophageal candidiasis, particularly those with multiple episodes, while taking into account the risk of resistant Candida strains developing. Suppressive therapy should also be considered for infants and children with severe, recurrent mucocutaneous candidiasis, especially if oesophageal candidiasis has occurred. Although many clinicians would not routinely recommend long-term prophylaxis against recurrent oropharyngeal or vulvovaginal candidiasis in people with HIV for the same reasons that routine primary prophylaxis is not advised, suppressive therapy may be considered in those with frequent or severe recurrences. Factors to weigh up include the effect of recurrences on wellbeing and quality of life, the need for prophylaxis against other fungal infections, cost, drug toxicity, drug interactions, and the potential for antifungal resistance in Candida and other fungi.
If long-term suppressive therapy as prophylaxis against mucocutaneous candidiasis is indicated in adults, adolescents, infants or children with HIV who have frequent or severe recurrences of oropharyngeal, oesophageal or vaginal candidiasis, the USPHS/IDSA recommends oral fluconazole as the treatment of choice and itraconazole oral solution as an alternative.
Long-term suppressive therapy to prevent recurrence or relapse of fungal infections in patients with HIV is generally continued for life. In some patients with HIV who had been receiving oral fluconazole to prevent recurrence of oropharyngeal candidiasis for a median of 18 months (range: 4-98 months) and were receiving effective combination antiretroviral therapy (about 50% had plasma HIV-1 RNA levels below the limits of detection), stopping oral fluconazole suppressive therapy led to recurrence of oropharyngeal candidiasis in only 10% of patients within 6-11 months. Although patients with HIV receiving suppressive antifungal prophylaxis may be at low risk of recurrence of fungal infections if their CD4+ T-cell counts increase to greater than 100/mm3 while receiving effective combination antiretroviral therapy, the USPHS/IDSA states that current data are insufficient to support a recommendation on stopping prophylaxis in these individuals.
Prevention of Fungal Infections in Transplant Patients and Patients with Cancer
Fluconazole is used prophylactically to reduce the incidence of candidiasis in patients undergoing bone marrow transplantation (BMT) who are receiving chemotherapy or radiotherapy. The medicine has also been used to prevent fungal infections in patients undergoing liver transplantation and in cancer patients considered at risk of neutropenia and fungal infections. There is some evidence that fluconazole prophylaxis in transplant and cancer patients can reduce the frequency of oropharyngeal and/or systemic candidiasis before neutrophil recovery. In addition, fluconazole prophylaxis may reduce the need for empiric antifungal therapy in these patients. The efficacy of oral fluconazole (400 mg once daily) for prophylaxis against fungal infections in neutropenic patients has been evaluated in a randomised, placebo-controlled study involving 274 cancer patients aged 18-80 years who were receiving cytotoxic chemotherapy or conditioning therapy for BMT. While the percentage of patients not requiring empiric therapy with IV amphotericin B was similar in both groups (57% of those receiving fluconazole and 50% of those receiving placebo required no such therapy), complete success without fungal colonisation was achieved in 37% of those receiving fluconazole and 20% of those receiving placebo. In addition, there was a lower incidence of superficial fungal infections in those receiving fluconazole (7%) than in those receiving placebo (18%), and only 3% of those receiving fluconazole developed definite invasive fungal infections compared with 17% of those receiving placebo. While fluconazole prophylaxis did not affect the overall mortality rate, intention-to-treat analysis indicates that the number of deaths attributable to definite invasive fungal infection was lower in the fluconazole group (1 of 15) than in the placebo group (6 of 15).
The use of primary antifungal prophylaxis in cancer patients undergoing myelosuppressive therapy or in patients undergoing BMT or solid organ transplantation remains controversial, particularly because such prophylaxis may predispose the patient to colonisation with resistant fungi and/or result in the emergence of highly resistant organisms. Retrospective studies have shown an increased risk of colonisation with Candida krusei in BMT recipients and in neutropenic patients who received fluconazole prophylaxis; in one study, about 41% of patients receiving fluconazole had colonisation with C. krusei compared with 17% of those not receiving fluconazole. Therefore, most clinicians generally discourage primary antifungal prophylaxis, except in certain carefully selected high-risk patients in whom the potential benefits are expected to outweigh the possible risks. Many experts, however, state that controlled, randomised studies should continue to evaluate fluconazole's use in preventing fungal infections in cancer patients and BMT recipients.
Dosage and Administration
Fluconazole is a triazole antifungal used for superficial mucosal (oropharyngeal, oesophageal or vaginal) candidiasis and fungal skin infections. It is also used for systemic infections, including systemic candidiasis, coccidioidomycosis and cryptococcosis. It has also been tried in blastomycosis, histoplasmosis and sporotrichosis.
Fluconazole is given orally or intravenously in similar doses. For intravenous infusion, it is given as a solution containing 2 mg/mL at a rate of 5 to 10 mL/minute (300 to 600 mL/hour). A maximum infusion rate of 100 mL/hour is recommended in the USA.
For superficial mucosal candidiasis (other than genital candidiasis), the usual dose of Fluconazole in the UK is 50 mg once daily by mouth. However, 100 mg once daily may be given if needed.
Treatment usually continues for 7 to 14 days in oropharyngeal candidiasis (except in severely immunocompromised patients), for 14 days in atrophic oral candidiasis associated with dentures, and for 14 to 30 days in other mucosal candidal infections, including oesophagitis. Higher doses are recommended in the USA, where an initial dose of Fluconazole 200 mg is followed by 100 mg once daily and where the minimum treatment period is 14 days for oropharyngeal infection, or a minimum of 21 days and at least 14 days after symptoms have resolved for oesophageal infections; doses of up to 400 mg once daily may be used for oesophageal candidiasis if necessary.
Oral Administration
Fluconazole may be taken by mouth with or without food. Fluconazole powder for oral suspension should be reconstituted when dispensed by adding 24 mL of distilled or purified water to the container holding 0.35 or 1.4 g of the drug to provide a suspension containing 50 or 200 mg/5 mL, respectively. The bottle should be shaken vigorously to suspend the powder; the suspension should be shaken well just before use.
IV Administration
IV infusions of Fluconazole should be given once daily at a rate not exceeding 200 mg/hour. Fluconazole injections for IV infusion should be visually inspected for discolouration and particulate matter before administration whenever the solution and container allow. The injection for IV infusion should be discarded if the solution is cloudy or contains a precipitate, or if the seal is not intact. Viaflex® Plus containers of Fluconazole should be checked for minute leaks by firmly squeezing the bag. The injection should be discarded if the container seal is not intact, leaks are found, or the solution is cloudy or contains a precipitate. Additives should not be introduced into the plastic injection container. The injection in plastic containers should not be used in series connections with other plastic containers, since this could result in air embolism from residual air being drawn from the primary container before administration from the secondary container is complete.
Fluconazole 150 mg as a single oral dose may be used for genital candidiasis (vaginal candidiasis or candidal balanitis). Dermatophytosis, pityriasis versicolor and Candida skin infections may be treated with Fluconazole 50 mg taken by mouth once daily for up to six weeks.
Systemic candidiasis, cryptococcal meningitis and other cryptococcal infections may be treated orally or by intravenous infusion with Fluconazole. The initial dose is 400 mg, followed by 200 to 400 mg once daily. The duration of therapy is based on clinical and mycological response, but it is usually at least 6 to 8 weeks. In cryptococcal meningitis in the USA, treatment is recommended for 10 to 12 weeks after the CSF cultures become negative.
Fluconazole may also be used in daily doses of 100 to 200 mg orally or intravenously to prevent relapse after a primary course of antifungal treatment for acute cryptococcal meningitis in patients with AIDS. In immunocompromised patients at risk of fungal infections, Fluconazole may be given prophylactically by mouth or by intravenous infusion at 50 to 400 mg once daily. However, long-term prophylaxis has been associated with the emergence of resistant organisms. Doses for children over 4 weeks of age are 3 mg/kg/day for superficial infections (a loading dose of 6 mg/kg may be used on the first day if necessary) and 6 to 12 mg/kg/day for systemic infections. A dose of 3 to 12 mg/kg/day may be given for prophylaxis in immunocompromised children. For infants under 2 weeks of age, all these doses should be given once every 72 hours. For those aged between 2 and 4 weeks, the doses should be given every 48 hours.
A maximum dose of 400 mg once daily should not be exceeded in children, or 12 mg/kg at appropriate intervals in infants. Dosage may need to be reduced in patients with renal impairment.
High Doses
Patients with life-threatening infections caused by Candida spp., Cryptococcus neoformans and Coccidioides immitis have been treated with doses higher than those recommended in the licensed product information for Fluconazole.
Dose-finding studies have found daily doses of 800 to 1000 mg of Fluconazole to be effective and well tolerated. In a study of 11 patients with HIV who received fluconazole 800 to 1000 mg once daily intravenously for 3 weeks, then orally until the CSF culture became negative, 6 patients had responded at 10 weeks, and another 2 improved clinically. Daily doses of up to 800 mg have been used in blastomycosis and coccidioidomycosis, and doses of 10 mg/kg/day have been tried in disseminated candidiasis.
Intermittent Doses
Concern has been raised about the increasingly widespread use of Fluconazole, particularly the impact of continuous fluconazole therapy in immunocompromised patients on the development of resistance. Nevertheless, Fluconazole remains popular for primary and secondary prophylaxis. Some investigators have suggested intermittent dosing, although this could further increase the risk of infections with resistant organisms. Once-weekly treatment with Fluconazole has been tried in onychomycosis and tinea capitis.
Administration in Renal Impairment
Patients with renal impairment may require a reduced dose. Normal loading or initial doses of Fluconazole should be given on the first day of treatment, and subsequent doses should be adjusted according to creatinine clearance (CC):
- CC more than 50 mL/minute: 100% of the standard recommended dose;
- CC less than 50 mL/minute and not receiving dialysis: 50% of the standard recommended dose;
- patients on regular haemodialysis: 100% of the standard recommended dose after each dialysis session. No dosage adjustment is needed in patients with renal impairment given single-dose therapy.
Adult Dosage
Oropharyngeal and Oesophageal Candidiasis
For treating oropharyngeal or oesophageal candidiasis, the usual adult dosage of Fluconazole is 200 mg as a single dose on the first day of therapy, followed by 100 mg or 200 mg once daily. Dosages up to 400 mg once daily may be used depending on the patient's response. Although clinical evidence of oropharyngeal candidiasis generally resolves within several days of starting fluconazole therapy, the manufacturer and some clinicians recommend that the drug be continued for at least 2 weeks to reduce the likelihood of relapse.

However, other clinicians question the need for prolonged therapy in patients with this infection. Patients with oesophageal candidiasis should receive fluconazole therapy for at least three weeks and for at least two weeks after symptoms have resolved. The optimal dosage for maintenance therapy in patients with oropharyngeal candidiasis has not been established. Oral doses of 50-100 mg once daily have generally been used effectively for maintenance therapy in these patients; doses of up to 200 mg once daily have occasionally been used.
Vulvovaginal Candidiasis
For the treatment of uncomplicated vulvovaginal candidiasis in non-pregnant women, the usual dosage of oral Fluconazole is a single 150-mg oral dose. For the treatment of recurrent vulvovaginal candidiasis in non-pregnant women, two 150-mg doses of oral Fluconazole should be given 3 days apart to achieve mycological remission. Then, a maintenance regimen of 100-150 mg once weekly should be given for 6 months to prevent recurrence. A 2-dose regimen of oral Fluconazole (two 150-mg doses given 3 days apart) is also recommended for the treatment of severe vulvovaginal candidiasis in non-pregnant women.
Leishmaniasis
Fluconazole has been tried in the treatment of cutaneous leishmaniasis caused by Leishmania major. In a randomised, double-blind, placebo-controlled study, 80 patients received a six-week course of oral Fluconazole 200 mg once daily, of whom 63 had complete healing of lesions after 3 months, compared with 22 of 65 patients who received placebo. However, others have reported a response rate that is not significantly different from placebo.
Other Candidal Infections
For treating systemic candidiasis, the usual adult dosage of Fluconazole is 400 mg as a single dose on the first day of therapy, followed by 200 mg once daily. In a limited number of patients with candidal urinary tract infections and peritonitis, doses of 50-200 mg once daily have been used. The optimum dosage and duration of therapy in patients with candidaemia, disseminated candidiasis and pneumonia have not been established; however, a limited number of such patients have received fluconazole doses of up to 400 mg once daily. Some clinicians have recommended that patients with invasive candidiasis receive Fluconazole in a dosage of 400-800 mg once daily. Therapy should be continued for at least 4 weeks and at least 2 weeks after symptoms have resolved.
Cryptococcal Infections
To treat cryptococcal meningitis, the usual adult dosage of Fluconazole is 400 mg as a single dose on the first day of therapy, followed by 200 to 400 mg once daily. Some evidence suggests that the 400-mg dosage is more effective than lower dosages in treating this infection. A higher dosage of Fluconazole (i.e. 800-1000 mg once daily) has been used in some patients with human immunodeficiency virus (HIV) infection for the treatment of cryptococcal meningitis. For initial therapy of cryptococcal meningitis, Fluconazole usually is continued for 10-12 weeks after the CSF is sterile.

Coccidioidomycosis
For treating coccidioidal meningitis in adults, fluconazole doses of 200-800 mg once daily have been recommended. For the treatment of coccidioidal meningitis in patients with AIDS, fluconazole doses of 400-800 mg once daily are recommended. Concomitant intracisternal, intraventricular or intrathecal amphotericin B therapy has been used in some patients.
Blastomycosis or Histoplasmosis
If Fluconazole is used to treat blastomycosis or histoplasmosis, a daily dosage of 400-800 mg is recommended.
Prevention of Fungal Infections in HIV-infected Individuals
In UK practice, routine primary prophylaxis against cryptococcosis in adults or adolescents with HIV infection and absolute helper/inducer (CD4+, T4+) T-cell counts less than 50/mm3 is not generally recommended.
While there is some evidence that oral Fluconazole given at 400 mg once weekly may be effective for primary prophylaxis against fungal infections in people with HIV infection, this regimen is not included in current UK guidance. Further study is needed to evaluate the efficacy of regimens other than daily administration for primary prophylaxis.
For long-term suppressive or maintenance therapy (secondary prophylaxis) of coccidioidomycosis in adults or adolescents with HIV who have had documented, adequately treated infections, a fluconazole dosage of 400 mg once daily is recommended by the USPHS/IDSA. For suppressive or maintenance therapy to prevent recurrence or relapse of cryptococcosis in adults or adolescents with HIV who have had documented, adequately treated infections, the usual dosage of oral Fluconazole is 200 mg once daily.
Some clinicians recommend that, for long-term suppressive therapy against cryptococcosis, oral Fluconazole be given at a dosage of 400 mg once daily for the first 4 weeks, followed by 200 mg once daily. If oral Fluconazole is used for long-term suppressive or maintenance therapy (secondary prophylaxis) to prevent recurrence or relapse of mucocutaneous candidiasis (oropharyngeal, vaginal, oesophageal) in adults or adolescents with HIV who have had frequent or severe episodes of these candidal infections, the USPHS/IDSA recommends a dosage of 100-200 mg once daily.
Although fluconazole has been given at a dose of 200 mg once weekly for long-term suppressive therapy in women with HIV infection and a history of oropharyngeal or vaginal candidiasis, this regimen is not included in current UK guidance. There are concerns that it could encourage the emergence of fluconazole-resistant strains of Candida. Long-term suppressive or maintenance therapy to prevent recurrence or relapse of fungal infections in patients with HIV infection is generally continued for life. However, UK specialist guidance indicates that it may be reasonable to stop suppressive or maintenance therapy for cryptococcosis in certain adults and adolescents who have had immune recovery as a result of effective combination antiretroviral therapy.
Prevention of Fungal Infections in Transplant Patients and Patients with Cancer
To prevent candidiasis in bone marrow transplant recipients, the recommended dose of fluconazole is 400 mg once daily. In patients expected to develop severe granulocytopenia (neutrophil count less than 500/mm3), fluconazole should be started several days before the expected onset of neutropenia. It should then be continued for 7 days after the neutrophil count rises above 1000/mm3.
Paediatric Dosage
The usual dose of fluconazole in paediatric patients ranges from 3-12 mg/kg once daily; doses above 600 mg daily are not recommended. The manufacturer states that a dose of 3, 6, or 12 mg/kg daily in paediatric patients is equivalent to 100, 200, or 400 mg daily, respectively, in adults. Some older children may have clearance similar to that of adults.
To treat meningitis or septicaemia caused by susceptible Candida, neonates and infants aged 3 months or younger have received fluconazole at a dose of 5-6 mg/kg once daily, given by mouth or by IV infusion over 1 hour. In some neonates and infants with septicaemia, an initial loading dose of 10 mg/kg was given, followed by 5 mg/kg once daily. Based on available pharmacokinetic data for fluconazole in premature neonates, the manufacturer recommends that neonates aged 2 weeks or younger receive the same daily dose as older children. However, the dose should be given once every 72 hours.
Oropharyngeal and Oesophageal Candidiasis
For the treatment of oropharyngeal or oesophageal candidiasis, the manufacturer recommends that paediatric patients receive 6 mg/kg of fluconazole on the first day, followed by 3 mg/kg once daily. The dose for oesophageal candidiasis may be increased to 12 mg/kg daily if needed, depending on the patient's condition and response to the medicine. Treatment for oropharyngeal candidiasis should continue for at least 2 weeks to reduce the chance of relapse. Treatment of oesophageal candidiasis should continue for at least 3 weeks and for at least 2 weeks after symptoms have cleared.
Other Fungal Infections
Fluconazole has been given at a dose of 6-12 mg/kg daily to treat systemic candidal infections in paediatric patients. The manufacturer recommends treating cryptococcal meningitis in paediatric patients with an initial dose of 12 mg/kg on the first day, followed by 6 mg/kg once daily. If needed, the dose may be increased to 12 mg/kg daily depending on the patient's condition and response to the medicine. Fluconazole should be continued for 10-12 weeks after the CSF becomes culture-negative.
Prevention of Fungal Infections in HIV-infected Individuals
The recommended oral dose of fluconazole for primary prophylaxis against cryptococcosis in HIV-infected infants and children with severe immunosuppression is 3-6 mg/kg once daily. If oral fluconazole is used for long-term suppressive or maintenance therapy to prevent recurrence or relapse of cryptococcosis or mucocutaneous candidiasis (oropharyngeal, oesophageal) in HIV-infected infants and children, the recommended dose is 3-6 mg/kg once daily. A dose of 6 mg/kg once daily is recommended for prophylaxis against recurrence or relapse of coccidioidomycosis in these paediatric patients.
Interactions
In general, fluconazole has fewer interactions than itraconazole or ketoconazole. Taking rifampicin with fluconazole reduces plasma concentrations of fluconazole. Hydrochlorothiazide taken with fluconazole has resulted in clinically insignificant increases in plasma fluconazole concentrations.
Fluconazole may interfere with the metabolism of some other drugs, mainly by inhibiting the cytochrome P450 isoenzymes CYP3A4 and CYP2C9. This may explain the reported increases in plasma concentrations of bosentan, ciclosporin, midazolam, nevirapine, amitriptyline, nortriptyline, phenytoin, rifabutin, sulfonylurea hypoglycaemics and nateglinide, selective cyclo-oxygenase-2 inhibitors such as celecoxib and parecoxib, tacrolimus, triazolam, warfarin and zidovudine. Fluconazole may inhibit the formation of a toxic metabolite of sulfamethoxazole. Increases in terfenadine concentrations after high doses of fluconazole have been associated with ECG abnormalities.
A similar effect may be expected with astemizole. However, using fluconazole with cisapride could increase cisapride concentrations and cause related toxicity, so this combination should be avoided. Fluconazole should also be avoided with astemizole, cisapride or terfenadine because of the risk of cardiac arrhythmias. Syncope was attributed to increased amitriptyline concentrations when amitriptyline was taken with fluconazole.
Fluconazole may also reduce the clearance of theophylline. Concentrations of contraceptive steroids have been reported as both increased and decreased in patients receiving fluconazole, and the effectiveness of oral contraceptives may be affected. For further information on interactions between drugs metabolised by the cytochrome P450 isoenzyme CYP3A and azoles, see under itraconazole.
Fluoroquinolones
Both levofloxacin and fluconazole can prolong the QT interval. The simultaneous use of intravenous levofloxacin and fluconazole resulted in an episode of torsade de pointes in a patient on haemodialysis.

Microbiological Interactions
A synergistic antifungal effect was seen in vitro with terbinafine and fluconazole against strains of Candida albicans.
Resistance
The emergence of strains of Candida spp. resistant to fluconazole has become increasingly important, particularly in immunocompromised patients receiving long-term prophylaxis with fluconazole. In addition to resistance in Candida albicans, infections with Candida dubliniensis, Candida glabrata and Candida krusei, all of which may be less sensitive to fluconazole than Candida albicans, have been noted in these patients. Secondary resistance of Candida glabrata has been reported during fluconazole therapy.
Resistance to fluconazole has been reported more often than resistance to ketoconazole or itraconazole, which may be related to the medicine's widespread use. Cross-resistance with other azoles and with amphotericin B has also been reported.
Fluconazole resistance has also been reported in Cryptococcus neoformans and Histoplasma capsulatum. Histoplasmosis developed during treatment with fluconazole in a patient with HIV infection. Fluconazole-resistant C. neoformans was isolated from an immunocompetent patient not previously exposed to azole antifungals.
Fluconazole Drug-Drug Interactions
Alfentanil
In a randomised, double-blind, placebo-controlled, crossover study in nine subjects, fluconazole 400 mg reduced the clearance of alfentanil 20 micrograms/kg by 55% and increased alfentanil-induced subjective effects.
Amitriptyline
An interaction between fluconazole and amitriptyline has been reported.
- A 12-year-old boy with prostatic rhabdomyosarcoma had episodes of syncope periodically over 7 months while taking fluconazole for chemotherapy-induced mucositis. He had taken fluconazole in the past without problems. However, he was also taking a stable dose of amitriptyline for neuropathic pain. After amitriptyline was withdrawn, he had no further episodes. The effect was confirmed by re-administration.
Concurrent administration of fluconazole probably increases exposure to amitriptyline. Three reports in adults have shown increased amitriptyline plasma concentrations with concurrent fluconazole use; in one patient, a 57-year-old woman, the QT interval was prolonged and torsade de pointes occurred.
Amphotericin
In vitro studies and animal experiments have given conflicting results about possible antagonism between the effects of fluconazole and amphotericin on Candida species. However, large randomised, double-blind comparisons of fluconazole with and without amphotericin for 5 days in non-neutropenic patients with candidaemia showed no evidence of antagonism, but did show faster clearance of the organism from the blood and a trend towards improved outcomes in those who received the combination.
Antacids
Fluconazole absorption after oral administration is not influenced by gastric pH; therefore, antacids such as co-magaldrox do not affect it.
Antihistamines
Using terfenadine with fluconazole can lead to dangerously high terfenadine concentrations, resulting in cardiotoxicity. It is suspected that the same may happen with astemizole.
Benzodiazepines
Twelve healthy men took part in a randomised, double-blind, four-way crossover study to determine the interaction between fluconazole and bromazepam. They received single oral or rectal doses of bromazepam (3 mg) after a four-day pretreatment with oral fluconazole (100 mg/day) or placebo. Fluconazole caused no significant changes in the pharmacokinetics and pharmacodynamics of oral or rectal bromazepam.
Fluconazole increased blood concentrations of midazolam and triazolam.
The effects of fluconazole (400 mg loading dose followed by 200 mg/day) on the kinetics of midazolam were studied in 10 mechanically ventilated adults receiving a stable infusion of midazolam. Concentrations of midazolam increased by up to four-fold after the start of fluconazole therapy; these changes were most marked in patients with renal insufficiency. During the study, the ratio of a-hydroxy midazolam to midazolam progressively fell. The authors concluded that in ICU patients receiving fluconazole, a reduction in the dose of midazolam should be considered if the degree of sedation increases.
In a study of the pharmacokinetics and pharmacodynamics of oral midazolam 7.5-15 mg, switching from inhibition of metabolism by itraconazole 200 mg/day to induction of metabolism by rifampicin 600 mg/day caused an up to 400-fold change in the AUC of oral midazolam.
Calcium Channel Blockers
Fluconazole enhanced the blood pressure-lowering effects of nifedipine by increasing its plasma concentrations in a 16-year-old patient with malignant phaeochromocytoma who was taking long-term nifedipine for arterial hypertension and was given fluconazole for Candida septicaemia.
Carbamazepine
Fluconazole can cause carbamazepine toxicity, presumably by inhibiting CYP3A4.
- A 33-year-old man on stable therapy with carbamazepine (400 mg three times daily) for a seizure disorder became stuporose due to carbamazepine toxicity after taking fluconazole 150 mg/day for 3 days. Withdrawal of both drugs resulted in a fall in carbamazepine concentrations (maximum concentration 25 µg/ml) and a return to the patient's baseline mental state. Carbamazepine was restarted, and the patient had no further side effects.
- Carbamazepine serum concentrations increased during concomitant fluconazole administration (400 mg/day) in a 38-year-old man.
Ciclosporin
Fluconazole can increase ciclosporin concentrations by inhibiting CYP3A4. Some studies recorded minimal or no effects, but others found increased ciclosporin concentrations. Differences in the dose and duration of fluconazole treatment may explain these discrepancies. For example, there was no interaction at a fluconazole dose of 100 mg/day, but high doses of fluconazole (400 mg/day or more) increased blood ciclosporin and tacrolimus concentrations.
The interaction between ciclosporin and fluconazole has been evaluated retrospectively in 19 kidney and pancreas/kidney transplant recipients. Both intravenous and oral fluconazole altered blood ciclosporin concentrations. Five subjects did not have a significant interaction, but 15 did. No patient had nephrotoxicity or transplant rejection related to antifungal therapy.
The effects of higher doses of fluconazole on ciclosporin immunosuppression have been investigated in six renal transplant patients in a prospective, unblinded, crossover study. Baseline renal function, ciclosporin AUC, Cmax, Cmm, fmax and clearance were compared with those 2,4 and 7 days after starting oral fluconazole at a dose of 200 mg/day. From day 8 onwards, the ciclosporin dose was reduced by 50%, and the above parameters were repeated on day 14. The results are shown in Table 1. On repeated-measures ANOVA, only the AUC and Cmax on day 4 of fluconazole were significantly higher than on day 0. There were no significant changes in ciclosporin clearance and fmax. The authors concluded that changes in Cmin may not be sensitive enough to detect the described interaction and suggested monitoring the AUC near day 4 of treatment to guide ciclosporin dose adjustments in all patients taking concomitant fluconazole.
Cimetidine
Fluconazole absorption after oral administration is not influenced by gastric pH; therefore, cimetidine has no effect.
Clarithromycin
The effects of fluconazole and clarithromycin on the pharmacokinetics of rifabutin and 25-O-desacetylrifabutin were studied in 10 patients with HIV infection who received rifabutin 300 mg once daily, together with fluconazole 200 mg once daily and clarithromycin 500 mg twice daily. Plasma rifabutin AUC increased by 76% when either fluconazole or clarithromycin was given alone, and by 152% when both medicines were used together. The authors concluded that patients receiving rifabutin with fluconazole or clarithromycin should be monitored for rifabutin-related adverse effects.
Cyclophosphamide
Cyclophosphamide is a prodrug that is metabolised by CYP450 enzymes to produce alkylating species, which are cytotoxic, and the extent of cyclophosphamide metabolism correlates with both treatment efficacy and toxicity. In vitro studies in six human liver microsomes showed that the IC50 of fluconazole for reducing 4-hydroxycyclophosphamide production was 9-80 µmol/l.
A retrospective study in 22 children with cancer looked at the potential interaction between fluconazole and cyclophosphamide. Children with an established profile of cyclophosphamide metabolism who were not receiving other drugs known to affect drug metabolism were selected; 9 were taking fluconazole and 13 were controls. Plasma clearance was significantly lower in patients taking fluconazole at the same time (2.4 versus 4.2 1/ hour/m. It is unclear whether this interaction is associated with reduced therapeutic efficacy of cyclophosphamide.
Doxorubicin
The effect of fluconazole on the plasma pharmacokinetics of doxorubicin has been investigated in a randomised crossover study in non-human primates. Fluconazole (10 mg/kg/day) was given intravenously for 4 days before doxorubicin (2.0 mg/kg intravenously). Pretreatment with fluconazole did not affect the pharmacokinetics of doxorubicin, and the incidence of severe neutropenia (absolute neutrophil count below 0.5 x 109/1) was higher with doxorubicin alone than with the combination of doxorubicin and fluconazole. Therefore, fluconazole does not appear to contribute to the marrow-suppressive effects of doxorubicin.
Flucytosine
Using fluconazole and flucytosine together may have an additive effect. This combination could help in the treatment of cryptococcal meningitis.
HIV Protease Inhibitors
The pharmacokinetic interaction between fluconazole 400 mg once daily and indinavir 1000 mg three times daily was evaluated in an 8-day placebo-controlled crossover study; no significant interaction was observed.
The effect of fluconazole on the steady-state pharmacokinetics of ritonavir and saquinavir has been studied in patients infected with HIV-1. They received the protease inhibitor (saquinavir 1200 mg three times daily, n = 5, or ritonavir 600 mg twice daily) alone on day 1 and then with fluconazole 400 mg on day 2 and 200 mg on days 3-8. The median increase in saquinavir AUC was 50%, and the median increase in Cmax was 56%. In contrast, fluconazole did not affect the disposition of ritonavir.
Methadone
An interaction between fluconazole and methadone (a substrate of CYP3A4, CYP2C9, and CYP2C19) has been reported.
While taking a stable dose of methadone, a 60-year-old man with advanced cancer developed respiratory depression 2 days after receiving intravenous fluconazole for refractory oral candidiasis. Intravenous naloxone reversed the respiratory depression.
In a randomised, double-blind, placebo-controlled study in 25 patients, fluconazole 200 mg/day increased methadone concentrations, but patients treated with fluconazole did not show signs or symptoms of significant narcotic overdose.
Omeprazole
Fluconazole absorption after oral administration is not influenced by gastric pH; therefore, omeprazole has no effect. Omeprazole is extensively metabolised in the liver by 5-hydroxylation and sulfoxidation reactions, catalysed predominantly by CYP2C19 and CYP3A4, respectively. Fluconazole is a potent competitive inhibitor of CYP2C19 and a weak inhibitor of CYP3A4. The effect of fluconazole on the pharmacokinetics of a single oral dose of omeprazole 20 mg was evaluated after a single oral dose of fluconazole 100 mg and after 4 days of oral administration of 100 mg/day in 18 healthy male volunteers. Fluconazole increased the Cmax and mean AUC of omeprazole and prolonged its half-life (2.59 versus 0.85 hours).
Oral Contraceptives
Fluconazole did not significantly alter the pharmacokinetics of ethinylestradiol or norgestrel, and the investigators interpreted this as suggesting that treatment with fluconazole in a user of oral contraceptives would not increase the risk of pregnancy. However, the study used a 50 mg dose of fluconazole, and experience with higher doses has shown different results.
In another study, fluconazole reduced the systemic availability of ethinylestradiol in an oral contraceptive, but the doses used were not reported.
In an open, crossover study of 10 young healthy subjects, fluconazole 150 mg increased the serum concentrations of ethinylestradiol 30-35 µg/day.
The potential pharmacokinetic interaction between fluconazole 300 mg once weekly and an oral contraceptive containing ethinylestradiol and norethindrone (Ortho-Novum 7/7/7; Ortho-McNeil Pharmaceutical Inc, Raritan, NJ) has been studied in a placebo-controlled, double-blind, randomised, two-way crossover study in 26 healthy women aged 18-36 years. During the first cycle, they took the oral contraceptive only. During the second cycle, they were randomly assigned to oral contraceptive + fluconazole or oral contraceptive + placebo. In the third cycle, they were given the alternative treatment.
Fluconazole caused small but statistically significant increases in the AUCo-24 of ethinylestradiol and norethindrone. Those given fluconazole experienced no treatment-related side effects.
It therefore appears that there is no threat of contraceptive failure because of concomitant fluconazole administration.
Phenytoin
Co-administration of fluconazole and phenytoin resulted in markedly higher phenytoin concentrations.
Rifamycins
The combination of rifampicin with fluconazole has insignificant effects.
Statins
The effects of fluconazole on plasma fluvastatin and pravastatin concentrations were studied in two separate randomised, double-blind, two-phase crossover studies. Healthy volunteers received oral fluconazole 400 mg on day 1 and 200 mg on days 2 to 4, or placebo. On day 4, they took a single oral dose of fluvastatin 40 mg or pravastatin 40 mg.
Fluconazole increased the plasma AUC and half-life of fluvastatin by 80% but had no significant effects on the pharmacokinetics of pravastatin. The mechanism of prolonged elimination of fluvastatin was probably inhibition of CYP2C9. In contrast, pravastatin does not appear to be susceptible to interactions with fluconazole and other CYP2C9 inhibitors.
Fluconazole's effect on the pharmacokinetics of rosuvastatin has been investigated in a randomised, double-blind, two-way, crossover, placebo-controlled study. Healthy male volunteers were given fluconazole 200 mg/day or matching placebo for 11 days; rosuvastatin 80 mg was co-administered on day 8. Plasma concentrations of rosuvastatin, N-desmethyl rosuvastatin, and active and total HMG-CoA reductase inhibitors were measured up to 96 hours after the dose.
Fluconazole increased the AUC and Cmax of rosuvastatin by 14% and 9% respectively. Limited data for the N-desmethylated metabolite showed that the Cmax fell by about 25%. Fluconazole did not affect the proportion of circulating active or total HMG-CoA reductase inhibitors accounted for by circulating rosuvastatin. Therefore, fluconazole produced only minor changes in rosuvastatin kinetics, which were not clinically relevant.
Sulfonylureas
Concurrent administration of fluconazole with tolbutamide resulted in increased tolbutamide concentrations.
- A 56-year-old HIV-positive patient with diabetes mellitus taking gliclazide 160 mg/day developed severe hypoglycaemia when treated with co-trimoxazole 480 mg/day and fluconazole 200 mg/day. The authors speculated that fluconazole might have inhibited gliclazide metabolism by inhibiting CYP2C9.
The effects of fluconazole and fluvoxamine on the pharmacokinetics and pharmacodynamics of glimepiride have been studied in a randomised, double-blind, crossover study in 12 healthy volunteers who took fluconazole 200 mg/day (400 mg per day, fluvoxamine 100 mg/day, or placebo once daily for 4 days. On day 4, they took a single oral dose of glimepiride 0.5 mg.
Fluconazole increased the mean total AUC of glimepiride to 238%, the peak plasma concentration to 151% of control values, and the half-life of glimepiride was prolonged from 2.0 to 3.3 hours. This was probably due to inhibition of CYP2C9-mediated biotransformation of glimepiride by fluconazole. However, fluconazole did not cause statistically significant changes in the effects of glimepiride on blood glucose concentrations.
Tacrolimus
Because tacrolimus is metabolised by intestinal and hepatic CYP3A4, medicines that inhibit CYP3A4 can reduce tacrolimus metabolism and increase tacrolimus blood concentrations.
The effect of Fluconazole on tacrolimus blood concentrations has been studied in eight liver transplant patients in whom prophylactic Fluconazole (200 mg/day) was stopped because of rises in hepatic transaminases, renal dysfunction or eosinophilia (n = 1 each). Calculated tacrolimus concentrations fell by 13-81% (median 41%) between the fourth and ninth days after Fluconazole was withdrawn. Tacrolimus blood concentrations should be monitored carefully, and the dose increased as needed after Fluconazole is stopped.
The interaction between tacrolimus and Fluconazole has also been evaluated retrospectively in 19 kidney and pancreas/kidney transplant recipients. Both intravenous and oral Fluconazole altered tacrolimus blood concentrations. Five people did not have a significant interaction, and 15 did. No patient had nephrotoxicity or transplant rejection related to antifungal therapy.
- A 17-year-old man with cystic fibrosis who took Itraconazole after a lung-liver transplant had high trough concentrations of tacrolimus despite the relatively low dose (0.1-0.3 mg/kg/day).
- A patient taking tacrolimus 0.085 mg/kg twice daily with itraconazole 200-400 mg/day developed ketoacidosis, neutropenia and thrombocytopenia, requiring both medicines to be stopped.
- A 34-year-old renal transplant recipient taking a stable regimen of tacrolimus and methylprednisolone was given itraconazole 100 mg twice daily for a urinary yeast infection. Taking Itraconazole at the same time led to a marked increase in tacrolimus trough concentrations on the second day of treatment (from 13 to 21 µg/ml) and a rise in serum creatinine, making a 50% reduction in the tacrolimus dose necessary.
When Itraconazole was stopped, its effect on tacrolimus kinetics took 12 days to reverse. The inhibitory effect of Itraconazole happened quickly, but it took much longer to wear off, which is important in clinical management. So, when Itraconazole and tacrolimus are used together, close monitoring of tacrolimus blood concentrations and careful dose adjustment are essential to help avoid toxicity.
Warfarin
Using Fluconazole and warfarin together has, in some cases, led to a prolonged prothrombin time.
Zidovudine
In vitro, the combination of Fluconazole with valproic acid inhibited zidovudine glucuronidation in human hepatic microsomes more than other drugs such as atovaquone and methadone.
Side effects
Read the indications for use if you want to order Fluconazole online.
Side effects reported with Fluconazole most commonly affect the gastrointestinal tract, including abdominal pain, diarrhoea, flatulence, nausea and vomiting, and taste disturbance. Other side effects include headache, dizziness, leucopenia, thrombocytopenia, hyperlipidaemias and raised liver enzyme values. Serious hepatotoxicity has been reported in patients with severe underlying diseases such as AIDS or malignancy. Anaphylaxis and angioedema have been reported rarely. Skin reactions are rare, but exfoliative skin reactions such as toxic epidermal necrolysis and Stevens-Johnson syndrome have occurred, more commonly in patients with AIDS.
Alopecia
Alopecia has occasionally been reported in patients receiving Fluconazole, especially with prolonged use.
Effect on electrolyte balance
Hypokalaemia was associated with Fluconazole in 3 patients with acute myeloid leukaemia.
Effects on the heart
QT prolongation and torsade de pointes have been reported rarely in patients receiving Fluconazole.
Effects on the liver
Although severe hepatic reactions to Fluconazole are rare, they have been reported, especially in patients with severe underlying diseases or hepatic dysfunction. Raised liver enzymes are common, and there have also been reports of jaundice. Hepatic necrosis has rarely been seen post-mortem in patients with severe underlying disease who had received Fluconazole. In one such patient, the hepatotoxicity was considered dose-dependent.

Hypersensitivity
Desensitisation has been carried out successfully in an AIDS patient who showed hypersensitivity to both Fluconazole and Itraconazole. Over seven days, gradually increasing oral doses of Fluconazole (starting at 5 mg daily) were given; after that, the dose was maintained at 400 mg daily. No adverse reactions were noted during the desensitisation period or in the three months before publication of the report.
Precautions
Before buying Fluconazole online, read information about the medicine.
Fluconazole should be used with caution in patients with impaired hepatic or renal function. Abnormalities in haematological, hepatic and renal function tests have been seen in patients with serious underlying diseases such as AIDS or malignancy. Cases of torsade de pointes and QT prolongation have been reported rarely, and caution is advised when giving Fluconazole to patients with proarrhythmic conditions. Teratogenicity has occurred in animals given high doses of Fluconazole, and its use is not recommended during pregnancy.
Breastfeeding
Fluconazole passes into breast milk and reaches concentrations similar to those found in maternal plasma. However, licensed product information does not recommend its use during breastfeeding. In one report, no harmful effects were observed in an infant exposed to fluconazole in breast milk for six weeks, apart from a slight increase in lactate dehydrogenase levels. In the UK, recommendations on breastfeeding should be guided by the product information and specialist clinical advice.
Pregnancy
High (toxic) doses of Fluconazole, Itraconazole and ketoconazole have been reported to be teratogenic in rodents.
Although there is limited information about the use of these drugs in human pregnancy, there is a report of a woman who took Fluconazole 400 mg daily throughout pregnancy and gave birth to an infant with severe craniofacial and limb abnormalities. The abnormalities resembled those associated with Antley-Bixler syndrome, a genetic disorder. However, a teratogenic effect could not be excluded.
Although prescription-event-monitoring studies of Fluconazole did not identify adverse effects on the fetus, congenital abnormalities have occurred in infants whose mothers were given high doses of Fluconazole for 3 months or more. Data collected by the manufacturer on 198 women exposed to Itraconazole during the first trimester of pregnancy indicated that the malformation rate in both exposed women and matched controls was within the expected baseline risk for the general population.
Nevertheless, the manufacturers recommend avoiding Fluconazole, Itraconazole and ketoconazole during pregnancy. Licensed product information states that doses of voriconazole equivalent to those used therapeutically are teratogenic and embryotoxic in rodents. Therefore, the manufacturer recommends avoiding voriconazole during pregnancy and that women of child-bearing potential use effective contraception during treatment.
Similar recommendations have been made for posaconazole. Other azole antifungals, including butoconazole, clotrimazole, econazole, miconazole, sulconazole, terconazole and tioconazole, are reported to be embryotoxic but not teratogenic in rodents given high doses. Many of these drugs are used topically or intravaginally, and systemic absorption from these routes of administration varies. While these drugs may not necessarily be contraindicated in pregnancy, these potential risks should be considered when choosing antifungal therapy for such patients.














